- The Yellow Bird
- Posts
- Retatrutide and the New Frontier in Weight Management
Retatrutide and the New Frontier in Weight Management
Discover the next frontier in weight management for women over 40. This newsletter explores how emerging therapies like retatrutide, a triple agonist targeting GLP‐1, GIP, and glucagon, are not only delivering unprecedented weight loss but also reducing systemic inflammation, improving joint health, and enhancing metabolic function. Tailored specifically for women navigating perimenopause and menopause, it breaks down the science behind these breakthroughs, offers practical strategies for integrating lifestyle and clinical support, and highlights actionable steps to reclaim energy, mobility, and confidence during midlife.
Why this isn’t just incremental progress, but a paradigm shift in treating obesity, metabolic dysfunction, and systemic inflammation
Over the past decade, weight‑loss pharmacotherapy has transformed from a niche diabetes treatment into a cornerstone of metabolic health care. With soaring prevalence of obesity and greater recognition of its link to cardiovascular disease, type 2 diabetes, joint degeneration, and chronic inflammation, medications that safely deliver significant, sustained weight reduction are urgently needed, especially for women over 40, who face unique physiological challenges due to hormonal shifts in perimenopause and menopause.
In this evolving landscape, retatrutide, a triple agonist targeting GLP‑1, GIP, and glucagon receptors, is emerging not just as another new drug, but as a potential paradigm shift, delivering unprecedented weight loss while also modifying inflammation and cardiometabolic risk in ways that extend beyond appetite suppression. Lilly Investor Relations+1
Current Pharmacotherapy: A Quick Comparative Overview
Clinical data show a clear gradient of efficacy among approved and emerging agents:
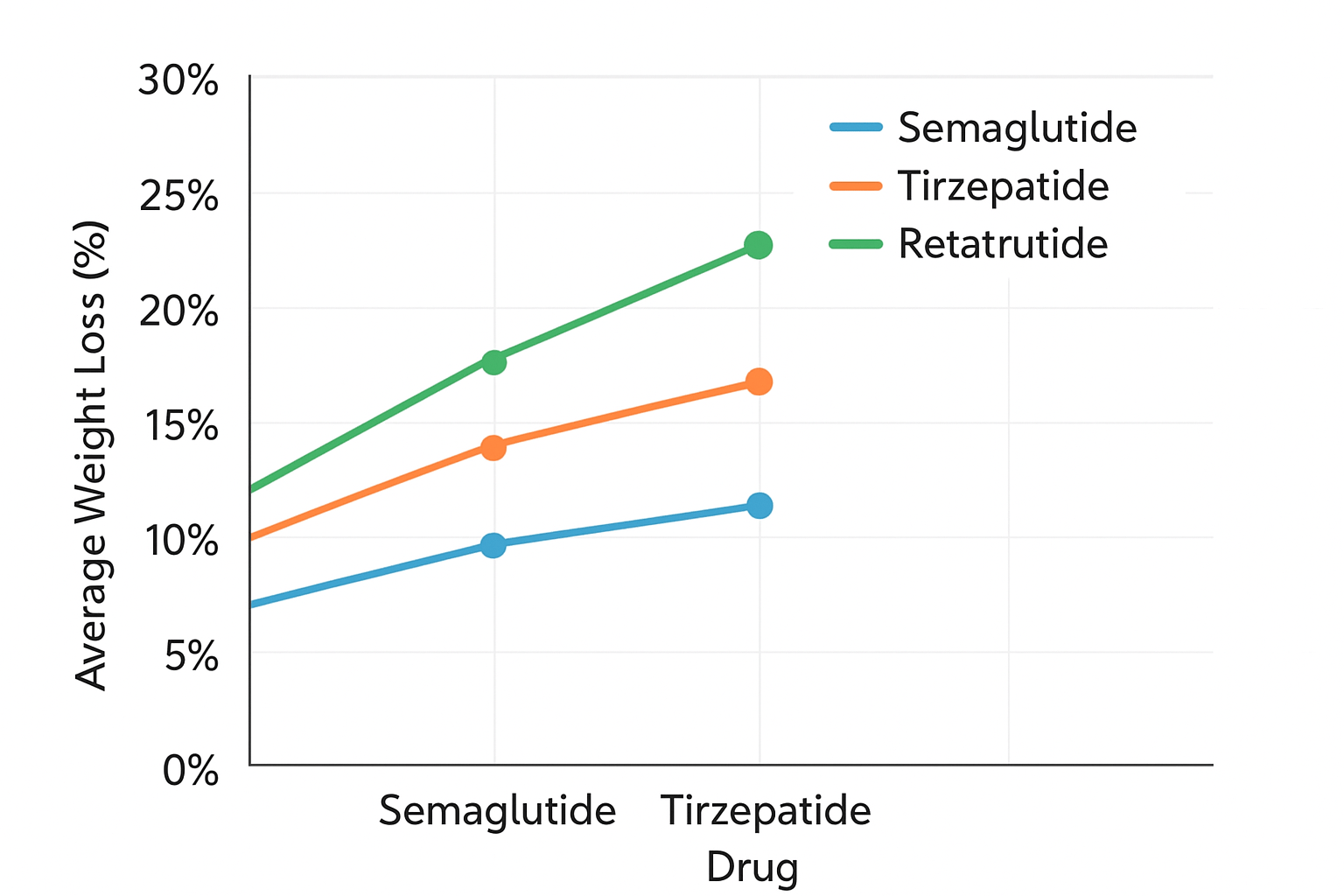
Semaglutide (Wegovy/Ozempic) , a GLP‑1 receptor agonist: ~15% average weight loss in obesity trials. Frontiers Publishing Partnerships
Tirzepatide (Zepbound/Mounjaro) , a dual GLP‑1 + GIP agonist: ~20–21% average weight loss. AP News+1
Retatrutide , GLP‑1 + GIP + glucagon triple agonist: Phase 3 results show up to 28.7% average body‑weight reduction over 68 weeks, along with marked improvements in joint pain, physical function, and metabolic biomarkers. Lilly Investor Relations+1
These differences are not trivial. They reflect fundamentally different biochemical effects and point to broader metabolic reprogramming, not just incremental improvements in appetite control.
Mechanisms of Action: Going Beyond Appetite Suppression
Understanding why retatrutide outperforms earlier drugs requires a review of the hormonal pathways involved:
1. GLP‑1 (Glucagon‑like Peptide‑1): Satiety and Glycemic Control
GLP‑1 receptor agonists like semaglutide mimic a gut hormone that:
Slows gastric emptying
Increases feelings of fullness
Improves insulin secretion and glycemic control
These effects reduce caloric intake and contribute to weight loss. Semaglutide and early GLP‑1 agonists helped define this class. Glucagon
2. GIP (Glucose‑dependent Insulinotropic Polypeptide): Enhancing Metabolic Efficiency
Tirzepatide added GIP agonism to the profile, which appears to:
Boost insulin sensitivity
Amplify GLP‑1’s effects through complementary signaling
Support lipid metabolism
This dual action drove tirzepatide’s step‑change in weight loss over GLP‑1 alone. Frontiers Publishing Partnerships
3. Glucagon Receptor Activation: Increasing Energy Expenditure
Retatrutide’s defining feature is glucagon receptor agonism, long understood in physiology to:
Stimulate hepatic glucose production
Increase lipolysis (fat breakdown)
Promote energy expenditure at the cellular level
In combination, these receptors help shift metabolism from “energy conservation” to fat utilization, particularly from visceral and hepatic fat, while maintaining balanced glucose control because GLP‑1 and GIP mitigate glucagon’s hyperglycemic potential. E-ENM
This triple axis, lowered appetite + improved insulin sensitivity + boosted energy expenditure, helps explain deeper and more sustained weight loss without relying solely on reduced food consumption.
Beyond Pounds: Inflammation, Pain, and Cardiometabolic Risk
A compelling aspect of the most recent Phase 3 data on retatrutide is its impact on inflammation and physical function, which is especially relevant for women over 40:
Reduced Pain and Improved Function
In adults with obesity and knee osteoarthritis, retatrutide significantly reduced:
Pain scores (WOMAC) by ~75%
Physical function impairment by a similar magnitude
~12–14% of participants completely pain‑free at Week 68
These changes are unlikely to be due solely to weight‑reduced mechanical load on joints; instead, they suggest modulation of inflammatory pathways as part of the treatment effect. PR Newswire
Reduction in Systemic Inflammation Markers
Retatrutide also lowered key markers of cardiometabolic risk and inflammation:
hsCRP (high‑sensitivity C‑reactive protein) , a sensitive marker of systemic inflammation
Triglycerides and non‑HDL cholesterol , linked to atherosclerotic risk
Blood pressure , a critical cardiovascular risk factor
These improvements provide evidence that retatrutide’s benefits extend well beyond weight alone, with meaningful implications for metabolic and cardiovascular health. PR Newswire+1
Why This Matters for Women Over 40
Women in perimenopause and menopause face specific biological and lifestyle challenges:
1. Hormonal Shifts Affect Fat Distribution
Estrogen decline shifts fat storage toward the abdomen, increases insulin resistance, and elevates cardiometabolic risk, changes that are resistant to diet and exercise alone.
2. Inflammation Rises with Age
Chronic low‑grade inflammation increases after menopause, contributing to joint pain, metabolic syndrome, and cardiovascular disease. Interventions that reduce systemic inflammation can therefore have outsized quality‑of‑life impacts.
3. Traditional Weight Loss Plateaus
Women often experience higher weight loss plateaus with traditional diet/exercise approaches due to changes in basal metabolic rate, muscle mass, and hormonal milieu.
A pharmacologic tool that addresses appetite, insulin sensitivity, energy expenditure, and inflammation targets these core factors simultaneously, offering holistic metabolic support rather than addressing only one piece of the puzzle.
Practical Guidance for Midlife Women
While pharmacotherapy is powerful, it is most effective when integrated into a comprehensive lifestyle strategy tailored to midlife physiology:
Evidence‑Based Recommendations
Lifestyle integration:
Protein‑rich diets to preserve lean mass
Resistance training to support metabolism
Adequate sleep and stress management to optimize hormonal balance
Clinical monitoring:
Lipid profile and hsCRP to track inflammatory change
Blood glucose and HbA1c for metabolic control
Blood pressure and cardiovascular risk assessments
Shared decision‑making:
Any medication, including novel agents like retatrutide, should be considered in consultation with a clinician familiar with your health history, goals, and risk profile.
Realistic Expectations and Safety
Despite strong efficacy data, retatrutide remains investigational and is not yet widely approved for general use. Common side effects seen in clinical trials are similar to other incretin‑based therapies:
Gastrointestinal symptoms (nausea, diarrhea, vomiting)
Reduced appetite
Less commonly, transient sensory sensations (e.g., dysesthesia) Lilly Investor Relations
These effects are generally manageable and often diminish with dose titration.
Take Action:
Join our live webinar on December 17 to learn more about how advanced weight-loss therapies like retatrutide can be integrated into lifestyle strategies for midlife women. Become part of our women-only Skool community for ongoing support, expert guidance, and peer accountability. Empower your health journey with knowledge, tools, and a supportive community that understands the unique challenges of midlife.
Retatrutide represents more than an incremental improvement over existing therapies; it embodies a mechanistically distinct and clinically powerful approach to weight management. By engaging three hormonal pathways, it delivers superior weight reduction while simultaneously targeting systemic inflammation, metabolic risk factors, and musculoskeletal pain, making it particularly relevant for women over 40 navigating midlife metabolic shifts.
For clinicians and patients alike, the emerging data illuminate a future where obesity treatment is precision‑oriented, multifactorial, and deeply aligned with each patient’s physiology and lived experience, a paradigm shift grounded in science, not buzzwords.
Here are our recommended resources:
Work With Me
If you want to explore peptide therapy within a structured, evidence-informed framework:
Find Me Here:
Here to plan with you, safely and effectively,

Disclaimer: This content is for educational purposes only and should not replace individualized medical guidance. Peptide therapy requires clinical oversight. Always consult a qualified healthcare provider before starting any treatment.